The ethics of incarceration have been debated since the eighteenth century, when public execution and torture were also broadly discussed. Mental illness—its social impact, treatment, and management—is closely tied to issues of criminal justice.[1] Modern prison systems in Europe and the United States have developed alongside response to mental illness, sometimes in parallel and sometimes in theoretical opposition to public and professional discourses about rehabilitation and punishment of mentally normal persons. Only in the past sixty years, however, has mental illness been medically investigated and medical treatment adapted to different conditions. In earlier periods the identification of mental illnesses was relatively unsophisticated, embracing successive theories of its causes and management. Many of those paradigms have now been now cast aside. Today diagnostic processes are, at least purportedly, based on carefully collected clinical evidence. Even though overall assessments of persons exhibiting signs of mental illness have improved, however, misdiagnosis continues to be a pitfall of contemporary treatment protocols. Therefore, although it may appear that the management of mental illness in the prison system has improved, evidence presented here suggests that there has been little progress.
When asked how the definition of mental illness has changed over the years, Colorado College Professor of Psychology Kristi Erdal joked in response, “How long do you have?” The definition and management of mental illnesses have changed over the past century so much that the complexity of historical diagnosis and treatment are difficult to summarize. In the late 1800s and early 1900s a patient was admitted to the insane asylum or psychiatric institute for essentially any crisis of behavior or personal circumstance: domestic trouble, religious excitement, opium addiction, intemperance, heredity, old age, and epilepsy.[2] The Colorado State Insane Asylum (later known as the Colorado State Hospital) was built in Pueblo in 1879 to house these individuals. Alcoholism was the primary diagnosis for the vast majority of those from the Front Range, plains, and intermountain Colorado region sent to the insane asylum in late nineteenth and early twentieth century. Alcohol abuse remained a frequent diagnosis in the 1940s and 1950s. The early hospital accepted the “better safe than sorry” perspective on institutionalization by admitting anyone who seemed to have behavioral problems.
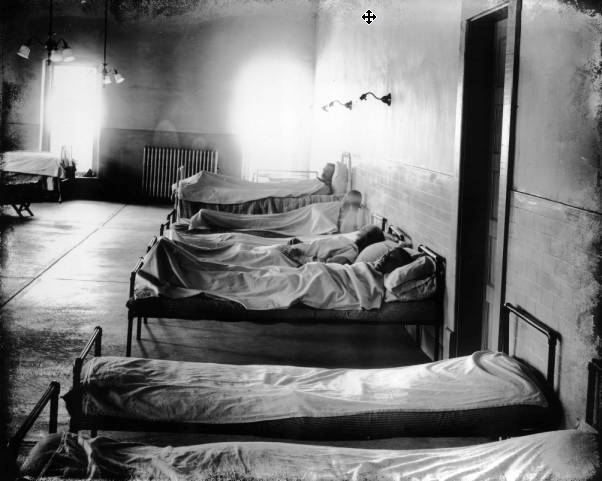
Because the early twentieth-century medical community and a society widely informed by physicians’ professional perspective envisioned an extensive array of mental illnesses, so many patients entered in the 1930s that the state mental facility in Pueblo was extremely overcrowded. Although its original construction anticipated a capacity of 2500 patients, the hospital in fact housed about 4000, most of whom had no criminal convictions.[3] Hospital beds overflowed into the hallways and disease spread rapidly. An outbreak of influenza in 1928 affected 321 patients; twenty died.[4]
Although epidemics of influenza and meningitis were exacerbated by overcrowding, patients at CSH who were psychically healthy enough to escape bodily illness and death were met with numerous rehabilitation programs. In the 1930s, hydrotherapy was an innovative technology. Occupational rehabilitation locations such as a dairy farm, laundry room, upholstery and sewing shop, and a metal shop were incorporated into the daily lives of the mental patients in the Pueblo facility. Special diets were also taken into account during mealtime, and the patients received adequate outdoor time on free grounds.[5]
Diagnosing mental illness
A major change in the interpretation of mental illness came with the introduction of the first Diagnostic and Statistical Manual of Mental Disorders (DSM) in the 1952. The DSM—a professional resource still published in successive editions—defines various mental illnesses, offering specific symptoms for each. “It is basically a flowchart that doctors use to diagnose,” claims Erdal. This flowchart-type diagnostic manual, along with certain legal regulations, required juries addressing criminal matters to consider only psychotic illnesses as relevant to criminal convictions. Schizophrenia, brief psychotic disorder, and other disorders that involve hallucinations are generally considered to be psychotic. In order for a jury to find someone not guilty by reason of insanity, his/her defense must demonstrate that at the time the crime was committed, the suspect experienced one of the psychotic illnesses and experienced a break from reality. This psychological state is extremely hard to determine, Erdal notes. Dr. Carl Bauer, who was interviewed by the Colorado Springs Gazette Telegraph in 1982, stated,
[A criminal] could have been crazy as hell, but if he intended to rape, that is mental illness, but not insanity. Insanity has to do with his mental condition, just preceding, not after the crime. People become crazy sometimes after the crime, particularly normal people, they disintegrate. It is called transient stress disorder. Under the stress of the incarceration they break down. But that has nothing to do with the mental illness that just preceded the crime that interfered with his ability to know that was a crime.[6] This distinction between milder mental illness and full-blown insanity remains elusive in the twenty-first century, so that many convicts who might in other periods or under other circumstances have been consigned to a mental institution instead go to prison.
A recent, troubling example of a judgment and conviction involving a mentally ill offender in Colorado is the case of James Holmes, the graduate student convicted for the Aurora Colorado theater shooting that left seventy injured and twelve dead. Two court-appointed psychiatrists examined Holmes and concluded that he did indeed have a mental illness, specifically paranoid schizophrenia, but claimed Holmes “was still able to know his actions were wrong.”[7] The jury determined Holmes to be legally sane at the time of the shooting, determining that his illness did not affect his decisions at the time of the shooting. Yet Holmes’ thought process at the time of the event is extremely difficult, if not impossible, to determine. Maybe he was sane at the time of the shooting, but maybe a schizophrenic episode provoked the entire event. Instead of receiving therapy and possibly treatment for his illness, James Holmes will now spend the rest of his life in a maximum-security prison without any form of rehabilitation. His case signposts for medical, judicial, and corrections communities in Colorado—as well as a general public transfixed by the details of this mass shooting and its sequel—that it is difficult to balance criminal justice and the human rights of the insane. Many victims and their families want Holmes to rot in a cell or even receive the death penalty: “an eye for an eye.” The jury disregarded any signs of a mental illness that may have provoked this action, perhaps to insure justice would be served.
If a mentally ill individual convicted in a legal process is lucky enough to avoid prison and go straight to a mental institution, he may find that the conditions there are not much different from those in prisons for the ostensibly sane. Public mental institutions often mimic prisons. With the constant problems of overcrowding and underfunding, sometimes the best they can do is warehouse the mentally ill and keep them at a safe distance from those who are mentally healthy.
The number of patients in the Colorado State Hospital in the 1930s and 40s was about 200 to 300. Today, the asylum—now called the Colorado Mental Health Institute at Pueblo (CMHIP)—holds more persons with criminal convictions than those without and has been criticized for treating patients unjustly.[8] A 1999 class action suit, Neiberger v. Hawkins, “alleged that the patients were being warehoused and given inadequate treatment. Therefore, some patients were being kept unfairly at the hospital longer than they would have served in prison for their crimes.”[9] Spearheaded by patients involuntarily committed to the forensic unit at CMHIP, the suit ended with many modifications to the hospital including a promise to increase individual therapy. The state checked in on the hospital for eighteen months after the suit, but only returned sporadically after that, so it is hard to determine if the new standards have been properly applied.[10]
Landmark court decision
A potential turning point in the treatment of mental illness among incarcerated offenders arose in the Pennsylvania Department of Corrections v. Yeskey case in 1998. In this case, the United States Supreme Court ruled that the Americans with Disabilities Act applies to state prisons as well.[11] The act essentially prohibits discrimination of disabled peoples in all aspects of life. The weakness of ADA with respect to the insane, especially insane criminal offenders, is that it does not necessarily protect the incarcerated persons from being poorly treated; it simply declares their rights to be equal to mentally stable offenders’. Pennsylvania DOC v. Yeskey thus appears to be a promising precedent for better management of mental illness among a prison population. Some of its stipulations are as follows:
- Prison officials are not required to provide accommodations that impose “undue financial and administrative burdens” or require “a fundamental alteration in the nature of [the] program.
- Prison officials are also allowed to discriminate if the disabled inmates’ participation would pose “significant health and safety risks” or a “direct threat” to others.
- Finally, some courts have said that prison officials can discriminate against disabled prisoners as long as the discriminatory policies serve “legitimate penological interests.”[12]
Evidently, however, discrimination in the discretion of the correctional officers is problematic. Numerous cases show correctional officers abusing their power over prisoners. One of many potential abuses is officers’ ability to place any prisoner in solitary confinement without review.
Execution of mentally ill offenders
Doctors, psychiatrists, and prisons’ reports and assessments, like the psychiatric reports in James Holmes’ case, have been constructed according to changing standards throughout the past century, as specific case studies show. One striking instance is Ed Hager’s 1909 case. Hager was put on death row for the murder of Elizabeth James. The city record stated, “Hager readily answers any questions asked him, but appears to have no curiosity to know what is going on in the outside world.”[13] The insanity experts at the trial said that Hager was sane at the time of the killing but that “possibly exposure and hunger, had afterwards temporarily upset his mental balance” as he was noticeably deranged walking around Pueblo after the murder. Hunger was the real etiology of record for this offender’s disturbed mental state.[14] But an early twenty-first century view might have been that Hager experienced a break from reality and should have been admitted to a room in a psychiatric institution. Instead he was admitted to a cell on death row.
In 1919, Cruz Romero occupied a cell on death row. His mentality was described as “abnormally dull, has never been developed and his mind is like that of an untaught child,” yet he was never sent to a hospital and never tested for sanity or mental insufficiency.[15] Ten years later, in 1929, Alberto Sanchez was evaluated on five separate occasions by doctors to test his mental state after being hospital-confined many times during his sentence. Each time the doctors reached a diagnosis of sanity. This “sane” man then proceeded to kill a fellow inmate.[16]
Frank Bailey, a prisoner on death row in 1939, was found insane following his trial and was known for being violent. Bailey actually spent time in the hospital for his illness, but was then transferred to the prison for being too violent for the mental hospital to manage.[17] Transferring a violently insane person to death row is contradictory to contemporary rehabilitative principles, but in the thirties Bailey remained in a non-medical corrections facility and continued to exhibit disruptive behaviors until the day he was executed. Had Hager, Bailey, or many individuals like them been alive today, perhaps they would have been admitted and treated properly in a hospital; then again, maybe they would have the same fate as Mr. Holmes.
In 1981 a criminal named Darrell Howell was twice determined to be mentally ill by two separate doctors, but at his trial a Dr. Fairbanks said in his testimony that he was seventy-five to eighty percent sure of Howell’s sanity.[18] As a result, Howell was judged competent and convicted. Howell’s attorney, Dennis Hartley, then stated, “One of the things we are citing is the failure of the judge to rule insanity.”[19] Howell’s lawyers were skeptical of the judge and jury’s ability to properly assess the situation when it comes to mental illness. How is it possible for anyone except the perpetrator to truly know what was going through his head at the time of the crime?
The prison system in general and, according to the evidence assembled here, particularly the Colorado State Penitentiary at Cañon City, does not do an adequate job of responding to the needs of a mentally unstable criminal. The definition of mental instability is constantly being revised. The overcrowding of asylums and the overbearing, watchful eye of current institutions has historically made mental hospitals less effective than they might be. With the removal of occupational rehabilitation, state resources for mentally ill criminals are focused on medication rather than rehabilitative programs. The 1998 Supreme Court case preventing the discrimination of the disabled in prisons was a step in the right direction in terms of the management of mental illness; but more can still be done. Some breaches of human rights of the criminally insane are rooted in the assessments performed and reported by psychiatrists and doctors. The case studies outlined above suggest that the problems in diagnosis have not diminished over time. The treatment and management of mentally ill prisoners needs to be revisited to remediate human rights violations.
[1] Originally researched and drafted by Stephanie Kelly.
[2] Nell Mitchell, The 13th Street Review: A Pictorial History of the Colorado State Hospital (Pueblo: My Friend, The Printer, 2009), 8.
[3] Ibid..
[4] Ibid., 27.
[5] Ibid., 15.
[6] Glenn Urban, “Insanity Pleas Create Difficult Problems for Courts,” Gazette Telegraph, November 8, 1982.
[7] Jack Healy, “Jury Rejects Mental Illness Argument for James Holmes in Aurora Theater Rampage,” New York Times, August 3, 2015.
[8] “Court Approves Hospital Monitoring Pact in Inmate Care Suit,” Class Action Reporter, January 8, 2003.
[9] Ibid.
[10] Ibid.
[11] Pennsylvania Dept. of Corrections v. Yeskey, 524 U.S. 206 (1998).
[12] “Know Your Rights Legal Rights of Disabled Prisoners,” American Civil Liberties Union, November 5, 2012, accessed November 8, 2015, https://www.aclu.org/files/images/asset_upload_file735_25737.pdf.
[13] “Will Be Hung Sometime during the Week beginning August 15,” Canon City Record, August 12, 1909.
[14] Ibid.
[15] “2 Murderers at Pen Will Hang Week of July 20; One More Later,” Cañon City Record, July 10, 1919.
[16] “Colorado News Notes,” Pueblo Indicator, June 21, 1930.
[17] “Negro Slayer Goes Berserk at Colorado State Prison Monday,” Cañon City Daily Record, October 31, 1938.
[18] “Howell Attorney Files for New Escape Trial,” unattributed fragment, September 15, 1981, Royal Gorge Regional Museum, “Howell” folder.
[19] Ibid.